THCA Notes
Volume XXXI, Number 10
October 2016
This month’s Commitment to Care (C to C) is focusing on Antibiotic Stewardship; Get Ahead of the Curve with the Basics
One a Month Update
The One a Month website has been updated with information for Prescribers and Pharmacists as well as a NEW graph indicated the latest data point for the LS Antipsychotic measure.
Check it out by clicking on the One a Month graphic.
Dementia as a Primary Diagnosis Code for Billing
The following clarification was provided by HHSC.
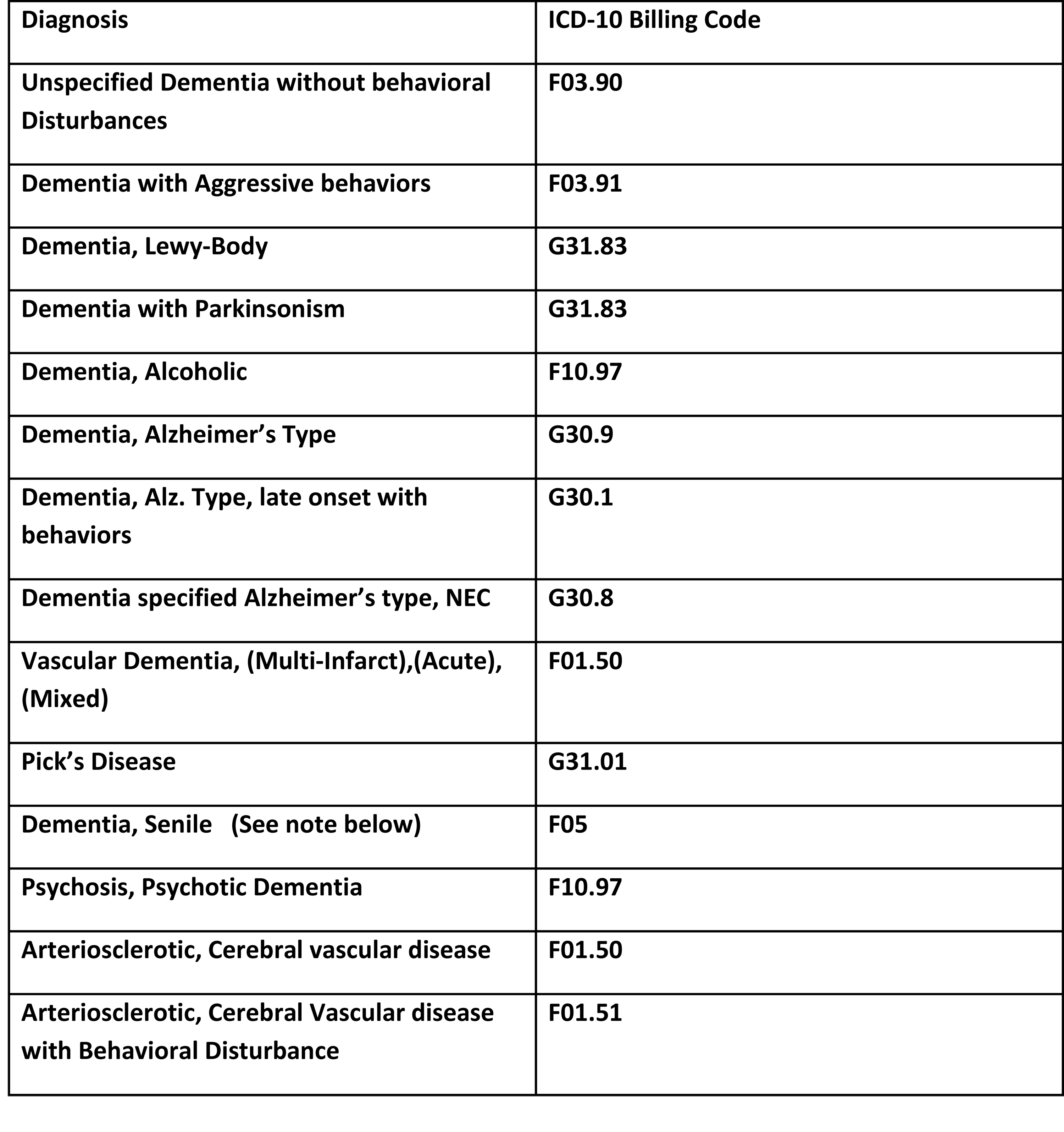
In order to use Dementia as a Primary Diagnosis, you must first ensure that the ICD-10 code is at the highest level of specificity as possible….the diagnosis may need to be further addressed by the attending physician. Below are the ICD-10 codes that are most commonly used for Residents with Dementia. TMHP has agreed that using the most specific codes available should prevent denials when claims are submitted for reimbursement.
- F05: Dementia, Senile includes the following conditions:
- Acute or subacute confusional state (nonalcoholic)
- Acute or subacute infective psychosis
- Acute or subacute organic reaction
- Acute or subacute psycho-organic syndrome
- Delirium of mixed etiology
- Delirium superimposed on dementia
- Sundowning
NEW MDS Mentor available, covers the following subjects:
- MDS 3.0 Updates: section GG and NPE
- Discharge Assessment Review
- Miscellaneous and FAQ
- Upcoming Training
- MDS News in Review
Access the September MDS Mentor Here
Lessons Learned from CMS
On September 29th, 2016 THCA met with CMS and other Stakeholder Associations and the following survey trends were shared.
INFECTION CONTROL – Gloving issues, sanitizing of shared glucometers and hand hygiene specifically in the dining room, when a staff member has repositioned a resident, etc. but doesn’t sanitize their hands prior to continuing to serve trays.
MEDICATIONS – Orders lacking clinical indication for use, no documentation on Pharmacy Recommendations related to why the physician has chosen not to follow the recommendation, and risk benefit for disregarding a black box warning. Lack of monitoring of behaviors or side effects for residents on medications for which the cited reason for the medication is to treat specific behaviors. Also lack of documentation for monitoring sleep for effectiveness of insomnia medications and anxiety for anxiolytics.
PAIN – Monitoring for effectiveness of analgesics especially during wound care. (stopping the treatment if the resident is obviously in moderate to severe pain, to evaluate and provide appropriate interventions prior to completing the treatment.
MDS CODING – Side rail assessment and coding related to whether the device is a restraint or not for the individual resident.
Whether you’re preparing your application for the AHCA/NCAL Quality Award or want to provide training for your staff on QAPI, below is a great resource for you and your staff.
AHCA/NCAL: QAPI News Brief Volume 1
Building Prevention into Every Day Practice: Framework for Successful Clinical Outcomes Series – Part 4 of 13
This is part of a series featuring one element of the Building Prevention into Every Day Practice: Framework for Successful Clinical Outcomes. The entire framework outlines key elements from both an organizational and clinical nature that are critical to successful clinical and organizational outcomes. Positively, these elements reflect common denominators that cross multiple care situations. Therefore, instead of being yet another initiative or single focused project to achieve just one outcome, it is a way of acting, thinking and being that will benefit multiple areas across an organization. Each element is addressed in detail throughout the framework.
This month THCA is featuring the element of Organizational Foundation: Team-Based Care
Key Takeaways: Team-Based Care
- No one discipline or individual can deliver all the necessary care and support.
- Create and reinforce a culture of giving care in the proper context of the “big picture” and not in “silos.”
- All departments and disciplines contribute and receive relevant information to help identify issues and concerns before they lead to a more complicated situation.
Visit the AHCA Clinical Practice website to learn more about the element of “Organizational Foundation: Team-Based Care” and answers to these key questions:
What does this mean? Why is this important? What are some examples? What is my part (as an individual employee, manager or practitioner)? What can my organization do?
Start somewhere, pick one element and work through it with your team.
Enjoy the journey through the framework!
“The Quality Initiative Series – Succeeding in the Midst of Change”
The AHCA Quality team is creating a series of FREE education Webinars which covers the best practices to help members with many of the new regulatory, payment or public reporting changes. The series is designed to provide critical support to members. It will consist of eight webinars and will start on July 27, 2016, 3 PM EST with a focus on rehospitalizations. You can register for the first webinar here.
The schedule is as follows:
November 16, 2016
3 – Unintended Healthcare Outcomes
January 25, 2017
4 – Staff Stability
April 26, 2017
5 – Antipsychotic Drug Reduction
June 21, 2017
6 – Functional Outcomes
September 20, 2017
7 – Customer Satisfaction/Experience
November 15, 2017
8 – Hospital Admissions in Long Stay Settings
President’s Report
Legislative Update
Commitment to Care
- Commitment to Care News – October 2016
State / THCA News
National / AHCA News
Education
- Stop Talking About Work/Life Balance! TEQ and the Millennial Generation
By Meagan Johnson